 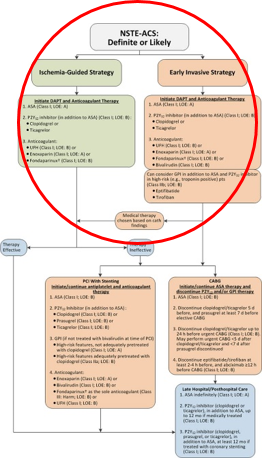 
10 – 12 Treatment of UA/NSTEMI in elderly patients is discussed in detail below.ĭespite the enormity of published information regarding the treatment of ACS, there is a paucity of data to guide the evaluation and management of ACS in the elderly, as only a minority of published clinical trials included elderly patients. This may be due to different culprit artery patency rates as well as different pathophysiological processes between STEMI and UA/NSTEMI, including differences in thrombus composition and mechanisms of ischemia. 1 Thrombolysis is contraindicated in UA/NSTEMI due to lack of benefit and increased risk of complications. Primary PCI is usually less urgent for UA/NSTEMI than in STEMI due to higher culprit artery patency rates and typically can be performed within 48 hours of symptom onset. In addition to standard ACS therapy, primary PCI is preferred in most UA/NSTEMI patients, especially those in higher risk categories. The ECG may be normal but may show ischemic changes, which include: new horizontal or down-sloping ST depression ≥0.05 mV in 2 contiguous leads and/or T-wave inversion ≥0.1 mV in 2 contiguous leads with prominent R/S ratio >1. The primary presenting symptom is ischemic chest pain (or equivalent). 7 – 10 Normal cardiac biomarkers are seen in UA which differentiates it from NSTEMI, which has elevated cardiac biomarkers. Unstable (UA) and and non-ST elevation myocardial infarction (NSTEMI) are grouped together as they are caused by incomplete occlusion of the culprit artery in 60% to 90% of cases. Unstable angina and non-ST elevation myocardial infarction Standard ancillary ACS therapy includes oxygen, antiplatelet agents (aspirin ± clopidogrel and/or glycoprotein IIb/IIIa inhibitors), nitrates, beta-blockers, anticoagulants (heparin, bivalirudin, or fondaparinux), and statins. 2, 3 The earlier the revascularization, the better the outcome (time is muscle). In addition to standard ancillary ACS therapy, the primary goal of treatment in STEMI, within 12 hours of symptom onset, is rapid revascularization with either thrombolysis in the absence of contraindications, or preferably, emergent percutaneous coronary intervention (PCI), when available. Cardiac biomarker values are often normal during the first few hours of STEMI. Revascularization should be initiated immediately based on the clinical presentation and ECG findings and should not be delayed until cardiac biomarker results are available. 2, 3Ĭardiac biomarkers are elevated in STEMI but are not necessary for the initial diagnosis. True posterior MI should be suspected when the ECG shows ST segment depression in leads V1 through V4 and can be differentiated from anterior ischemia by obtaining an ECG with posterior leads (V7 and V8), which reveals ST segment elevation in the presence of a posterior MI. STEMI also includes new or presumed-new left bundle branch block (LBBB), a finding more common in the elderly. 5, 6 STEMI is diagnosed in the presence of ischemic chest pain (or equivalent) when the ECG shows new ST-segment elevation at the J-point in 2 contiguous leads with the cut-off points of ≥0.2 mV in men or ≥0.15 mV in women, in leads V2 and V3 and/or ≥0.1 mV in other leads. ST-elevation myocardial infarction (STEMI) is caused by complete occlusion of the culprit artery in >80% of cases. 4ĪCS can be divided into two categories: ST-elevation myocardial infarction unstable angina and non-ST-elevation myocardial infarction. The 2007 Joint Task Force of the European Society of Cardiology, American College of Cardiology Foundation, the American Heart Association, and the World Heart Federation (ESC/ACCF/AHA/WHF) redefined acute myocardial infarction (MI) as the death of cardiac myocytes that is caused by ischemia and not by other etiologies such as inflammation or trauma. The electrocardiogram (ECG) and cardiac biomarkers (such as troponin) are useful for diagnosis and risk stratification and thus can guide treatment. Hemodynamic decompensation can occur due to ventricular arrhythmias or to severe myocardial dysfunction. Elderly ACS patients are less likely to present with typical symptoms as discussed in this article. The classical description is retrosternal chest discomfort that radiates to the jaw and left arm, which can be associated with dyspnea, diaphoresis, nausea, or vomiting. The clinical presentation of ACS is variable, but typically includes chest pain. If coronary blood flow is interrupted long enough, myocyte necrosis (infarction) can occur. ACS is most commonly caused by coronary atherosclerotic plaque rupture and subsequent intracoronary thrombus formation, which leads to myocardial ischemia. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
